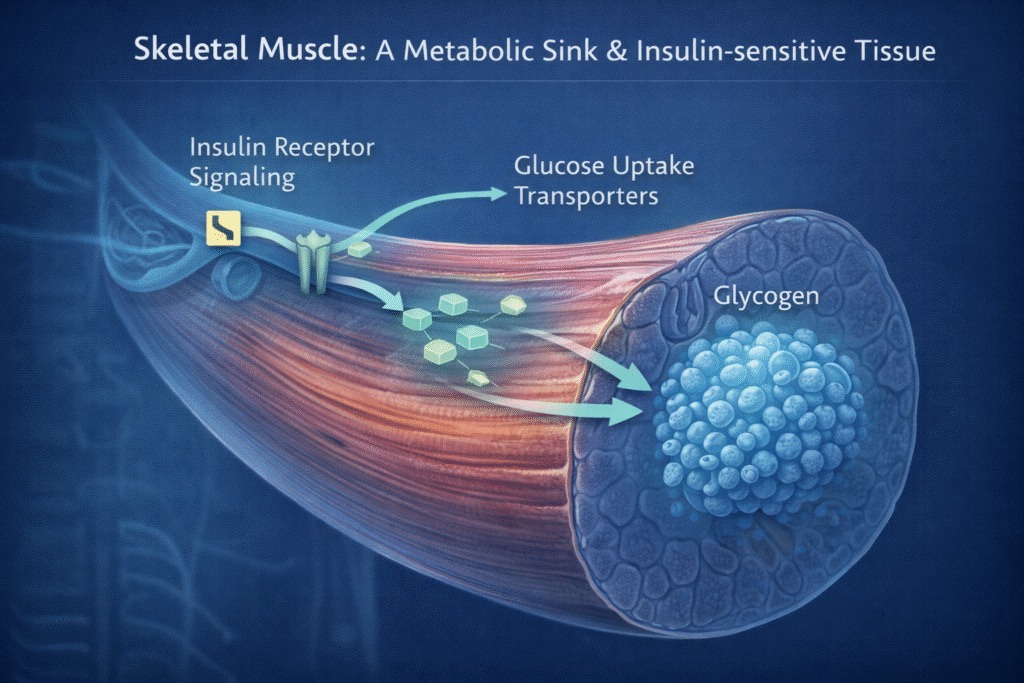
If you want to know how to improve insulin sensitivity, the answer begins with skeletal muscle — yet this is the most overlooked tool in conventional diabetes and prediabetes management. Muscle tissue is your body’s largest glucose disposal organ. Every kilogram of lean muscle you carry acts as a metabolic sink that absorbs glucose from your bloodstream independently of insulin. Which means building and preserving muscle is not just an aesthetic goal — it is one of the most direct biological interventions for insulin resistance available to you.
But here’s the twist: insulin is not the villain. In many cases, the real issue is that the body has lost enough metabolic infrastructure—especially healthy skeletal muscle—to handle carbs, stress hormones, sleep disruption, and modern living without glucose spilling over.
Think of muscle as your metabolic “storage and clearance engine.” When muscle function and mass go down, blood sugar problems get easier to trigger. When muscle goes up (and works better), metabolic health often becomes dramatically easier.
And this is where protein comes in—not as a trend, but as biology.
Key Takeaways
- Skeletal muscle is the principal tissue for insulin-stimulated glucose disposal, meaning it plays a central role in whole-body glycemic control. PubMed+1
- Resistance training improves insulin action in muscle and increases key proteins involved in glucose transport/signaling (including GLUT4). PubMed+1
- Adequate protein supports lean mass preservation, especially during fat loss—crucial for long-term metabolic stability. PMC+1
First, let’s stop demonizing insulin
Insulin is a hormone with a job: move nutrients into cells and coordinate storage, repair, and growth.
In a healthy system:
- insulin rises after meals,
- muscle takes up glucose efficiently,
- liver stores some glycogen,
- blood sugar returns to baseline.
In metabolic dysfunction, the problem is usually insulin resistance + overflow, not “insulin itself.” Your system is forced to push higher insulin to do the same job—especially when the tissues most responsible for clearing glucose (like muscle) aren’t doing their part well.
So instead of obsessing over “how to keep insulin low,” a smarter question is:
How do we rebuild the tissue that makes insulin work normally again?
Muscle is not aesthetics. It’s metabolic infrastructure.
Skeletal muscle isn’t just for movement. Metabolically, it’s one of the most important tissues you have.
Why?
1) Muscle is a major driver of glucose disposal
Skeletal muscle is widely described as the principal tissue for insulin-stimulated glucose disposal, making it a primary driver of glycemic control. PubMed+1
When muscle is insulin-sensitive, it can clear glucose efficiently. When it’s insulin-resistant (or when you don’t have enough of it), glucose stays higher for longer—and the whole system strains.
2) Muscle contraction has a “second doorway” for glucose
Even without insulin, muscle contraction (exercise) can increase glucose uptake. Then afterward, trained muscle becomes more insulin-sensitive—meaning the next meals are handled better.
This is one reason resistance training and walking are so powerful in type 2 diabetes and prediabetes: you’re not just burning calories—you’re improving tissue function.
3) Muscle is a “buffer” against metabolic chaos
When life hits (stress, poor sleep, travel, holidays), muscle gives you metabolic wiggle room. Less muscle = less buffer. More muscle = more resilience.
Healthy Pathway
Meal glucose
↓
Bloodstream
↓
Skeletal muscle (GLUT4)
↓
Glycogen / oxidation
↓
Stable blood sugar
Dysfunctional Pathway
Meal glucose
↓
Bloodstream
↓
Poor muscle uptake
↓
Liver
↓
Liver fat / high fasting glucose
Figure 1. When skeletal muscle is insulin-sensitive, glucose has somewhere to go. When it is not, overflow is redirected to the liver.
The biggest misconception: “Protein is bad because it raises insulin.”
Yes—protein can stimulate insulin somewhat. That’s not automatically bad.
Here’s what’s often missed:
Protein-triggered insulin can be physiologic
Insulin isn’t only about glucose. It also supports amino acid uptake and tissue repair. In many contexts, an insulin rise after protein is part of normal anabolic physiology.
The relevant question is: what happens to glucose after the meal?
For most people with metabolic dysfunction, the bigger problem is:
- poor muscle glucose uptake,
- excessive hepatic glucose output,
- elevated post-meal glucose peaks,
- and chronic inflammation/stress signaling.
Protein—especially when it helps preserve/build muscle—often improves the system long-term.
In other words: don’t fear the signal. Fix the tissue.
Resistance training: one of the fastest ways to improve muscle insulin action
If you do nothing else from this article, do this:
Strength train consistently.
Even modest programs have measurable effects.
A classic example: strength training ~30 minutes, three times per week improved insulin action in skeletal muscle and increased proteins involved in glucose transport and insulin signaling (including GLUT4). PubMed+1
This matters because you’re not just “getting stronger.” You’re changing your metabolic machinery.
What to do (simple and realistic)
You don’t need a perfect plan. You need consistency.
Option A (minimal effective):
- 2–3 days/week
- 30–45 minutes
- focus on large movements: squat pattern, hinge pattern, push, pull, carry
Option B (home version):
- split squat or goblet squat
- hip hinge (RDL pattern) or glute bridge
- push-ups or dumbbell press
- rows or band rows
- farmer carry
Progress slowly. Add reps. Add load. Add control. The body adapts.
Protein: the raw material for lean mass (especially during fat loss)
A lot of people lose weight and think they’re “fixing metabolism.” But if that weight loss includes significant muscle loss, they often end up with:
- worse long-term glucose tolerance,
- lower metabolic rate,
- and a fragile system that rebounds easily.
High-protein intake helps protect lean mass during weight loss
Research in humans shows that higher protein intake during diet-induced weight loss can attenuate declines in lean/muscle mass. PMC+1
This is especially important if someone is:
- in a caloric deficit,
- doing lots of cardio but little strength training,
- using appetite-suppressing approaches,
- or older (where muscle maintenance is harder).
Protein also tends to improve satiety and energy expenditure
Protein is generally more satiating and can support energy expenditure compared with lower protein patterns (mechanistically: higher thermic effect and other factors). PMC+1
The point isn’t “eat protein to burn calories.” The point is:
Protein makes fat loss less destructive and more sustainable.
How much protein do I actually need?
This depends on goals, age, and activity—but we can give sane ranges.
For exercising individuals, the International Society of Sports Nutrition has stated that ~1.4–2.0 g/kg/day is sufficient for most people training, with higher intakes sometimes useful during hypocaloric phases. PubMed+1
For older adults, multiple expert groups and analyses support higher-than-RDA protein to support lean mass, often around 1.0–1.2 g/kg/day minimum, and commonly higher with resistance training. ScienceDirect+1
Practical “Fix Metabolic Chaos” targets
- If you strength train: aim roughly 1.6 g/kg/day as a strong middle-ground starting point (adjust based on appetite, digestion, and results). PubMed+1
- If you’re older and want muscle maintenance: don’t flirt with the minimum—aim closer to 1.2–1.6 g/kg/day, especially if you train. ScienceDirect+1
Important note: If someone has significant kidney disease (especially advanced CKD), protein targets should be individualized with their clinician.
Timing: do you need “perfect protein timing”?
Not perfect. But distribution helps.
A simple rule:
- Get a solid protein “dose” 2–3 times per day, rather than one giant protein meal and the rest low-protein snacks.
If you’re strength training, having protein within a few hours around training is practical—not magic, just supportive.
The real metabolic blueprint (the 2-lever system)
If you want insulin sensitivity and stable glucose, the big levers are:
Lever 1: Build and maintain muscle
- Strength training 2–4x/week
- Daily movement (walking is underrated)
- Progressive overload over time
Lever 2: Feed muscle enough protein to adapt
- protein target that matches your physiology
- enough total energy and micronutrition to recover
- avoid “dieting yourself into sarcopenia”
When these two levers are pulled consistently, the physiology often shifts fast.
“Next, we’ll explore how the gut–liver axis influences insulin resistance.”
→ the gut–liver axis
Resistance Training
do resistance training
↓
high GLUT4 expression
↓
high insulin signaling efficiency
↓
high muscle glycogen storage
Adequate Protein
adequate protein intake
↓
supports muscle protein synthesis
↓
preserves lean mass during fat loss
↓
supports training adaptation
- Resistance training → ↑ GLUT4, ↑ insulin signaling proteins, ↑ glycogen storage
- Adequate protein → supports MPS/lean mass, protects muscle during fat loss
(Caption: “You’re not managing glucose with willpower. You’re upgrading tissue.”)
Action steps (do this for 14 days)
If you want an easy, real start:
- Strength train 3x/week (30–45 min)
Pick 4 movements. Keep it simple. - Walk daily (10–20 minutes after at least one meal)
This is one of the easiest “glucose hacks” that isn’t a hack. - Hit your protein target daily
Don’t “average it out.” Make it consistent. - Track one thing
Choose one:
- fasting glucose trend
- post-meal glucose response (if using CGM)
- waist measurement
- strength progress
Consistency beats complexity.
Disclaimer
This content is educational and not medical advice. If you’re on glucose-lowering medication (especially insulin or sulfonylureas), changes in diet/training can change your glucose needs—coordinate with your prescribing clinician.
About the Author
Morteza Ariana is a State-Certified Functional Nutritionist based in Germany, specializing in insulin resistance, type 2 diabetes, and root-cause metabolic restoration. He holds advanced training in systems-based physiology and has worked with patients across the U.S. and Europe for over 10 years.
His clinical framework is built around a core principle that mainstream medicine consistently overlooks: chronically elevated insulin — not blood glucose — is the earliest and most actionable driver of metabolic disease. That conviction was shaped in part by his own experience with hyperinsulinemia in 2016, and deepened through a decade of clinical practice and the study of leading researchers in metabolic medicine including Benjamin Bikman, Joseph Kraft, Gerald Reaven, Jason Fung, and Stephen Phinney.
His work focuses on identifying and correcting the upstream metabolic signals — insulin load, liver-gut axis dysfunction, circadian misalignment, and micronutrient gaps — that standard screening misses entirely. Patient outcomes are documented, anonymized, and published on this site.
If this resonates, the next step is clarity
The Metabolic Restoration Blueprint is a structured 12-week framework designed to correct upstream metabolic drivers — not just manage symptoms.
References (science-forward, not media)
- Skeletal muscle as principal tissue for insulin-stimulated glucose disposal / driver of glycemic control. PubMed+1
- Strength training improves insulin action and increases GLUT4 and insulin signaling proteins in skeletal muscle. PubMed+1
- Higher protein intake during weight loss attenuates lean mass loss (and related evidence). PMC+1
- ISSN position stand: daily protein intake ranges for exercising individuals. PubMed+1
- Protein needs for older adults (expert recommendations). ScienceDirect+1
