What Conventional Care Will Not Tell You About Reversing Type 2 Diabetes
The patient who walks into my practice asking whether type 2 diabetes can be reversed has almost always been told for years that it cannot. The conversations they remember are about disease management, medication titration, and learning to live with a chronic, progressive condition. The conversation they have rarely had is about why the diabetes developed in the first place, whether the conditions that produced it can be removed, and whether insulin sensitivity can be restored. The framing they were given was clinical custody, not clinical curiosity.
Can type 2 diabetes be reversed? In a meaningful fraction of patients, yes — and the clinical reality is more hopeful than conventional care typically communicates. Reversal is not promised, it is not guaranteed, and it does not look the same in every patient. But the underlying biology of type 2 diabetes — chronic carbohydrate overload, hyperinsulinemia, visceral fat, fatty liver, poor sleep, stress physiology, low muscle mass, and mitochondrial dysfunction — is in many cases addressable, and when those drivers are systematically corrected, a substantial proportion of patients move from active diabetes to functional remission.
This post is a clinical synthesis of what I have learned in over a decade of working with type 2 diabetes patients in functional medicine practice — what reversal actually looks like, what the typical 12-week trajectory is, what determines who fully reverses and who improves significantly without full remission, the dietary protocol I use, how medications come down in coordination with the GP, and the increasingly relevant question of GLP-1 drugs in this context.
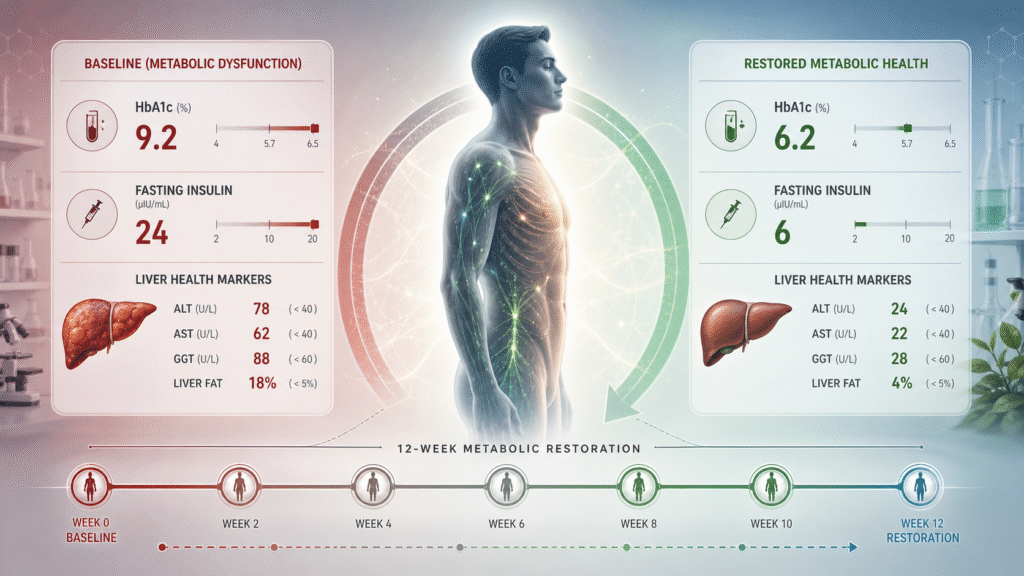
Documented patient outcomes — including HbA1c reversals from 10.5 percent to 6.2 percent, and from 9.2 percent to 6.5 percent, with insulin and oral medications discontinued or reduced — are published on the documented outcomes page and referenced throughout this post.
What you will learn: What “reversal” of type 2 diabetes actually means clinically | The biological mechanism that makes reversal possible in many patients | The 12-week trajectory of metabolic restoration, week by week | Why some patients reach full remission and others achieve significant improvement without remission | The dietary protocol I use for newly diagnosed versus long-term insulin-dependent patients | The GLP-1 question: how I integrate Ozempic, Mounjaro, and similar drugs into a reversal framework
What Reversal Actually Means
The first conceptual point that has to be established is what “reversal” means and does not mean. The medical literature now uses the term “remission” — a state in which HbA1c remains below 6.5 percent without glucose-lowering medication for at least three months. This is the term most international diabetes societies have converged on, and it is the framework I use clinically.
Remission is not cure. The underlying susceptibility to type 2 diabetes does not vanish — the metabolic vulnerability that allowed the disease to develop the first time can be reactivated by returning to the conditions that created it. A patient who achieves remission and then resumes the dietary, sleep, and lifestyle pattern that produced their original diabetes will see the disease recur. Remission is the restoration of normal glucose regulation through restoration of underlying physiology. Cure would be permanent immunity. Those are different things, and patients deserve clarity on the distinction.
What remission does mean is profound. It means HbA1c in the non-diabetic range without medication. It means fasting glucose normalized. It means the patient is no longer experiencing the progressive trajectory of complications that diabetes produces — the cardiovascular damage, the kidney decline, the retinopathy risk, the neuropathy risk.
It means a different long-term life expectancy and quality of life. Even when full remission is not achieved, the partial reversal that many patients experience — substantial improvement in HbA1c, fasting insulin, triglycerides, hepatic markers, and visceral fat, with significant medication reduction — is itself a clinically meaningful outcome that changes the long-term trajectory of the disease.
The framework I use with patients is straightforward: the body can often recover far more than conventional medicine suggests, but recovery exists on a spectrum. The goal is not perfection. The goal is restoring physiology, reducing disease burden, improving metabolic flexibility, and reclaiming function. Within that goal, full remission is one outcome among several that are all worth pursuing.
The Biological Mechanism: Why Reversal Is Possible
Type 2 diabetes, as conventionally diagnosed, is the late stage of a process that has typically been developing for ten to twenty years before it shows up on a glucose panel. The early stages are insulin resistance and hyperinsulinemia — the body producing more insulin to maintain glucose at acceptable levels in the face of declining insulin sensitivity at the cellular level. During this prolonged compensatory phase, fasting insulin is elevated while fasting glucose and HbA1c remain in ranges that conventional screening calls normal. The patient is metabolically ill but not yet diagnosable by the standard panel.
The transition to overt type 2 diabetes occurs when the pancreatic beta cells can no longer produce enough insulin to overcome the peripheral insulin resistance and overcome the elevated hepatic glucose output. Glucose rises, HbA1c crosses 6.5 percent, the diagnosis is made, and medication is initiated. By this point, the underlying drivers — visceral fat, fatty liver, chronic dietary carbohydrate overload, sleep and circadian disruption, sarcopenia, and chronic inflammation — have been operating for years.
The reason reversal is biologically possible in many patients is that most of these underlying drivers are reversible. Visceral fat responds to dietary and metabolic intervention. Fatty liver clears within weeks of reducing hepatic fat synthesis through dietary carbohydrate restriction. Hyperinsulinemia normalizes when insulin demand drops. Beta cell function, when not yet exhausted, recovers significantly when the chronic glucose and insulin pressure is removed.
The cellular insulin signaling machinery is plastic — when the conditions producing insulin resistance are removed, sensitivity often returns. The patient is not locked into the disease state. They are inhabiting a metabolic state that the body produced in response to chronic conditions, and when those conditions change, the state changes with them.
The variable that determines whether reversal is biologically possible for a given patient is largely residual beta cell function. Patients in the first few years after diagnosis typically retain substantial beta cell capacity — the cells are stressed but not exhausted. Patients who have had advanced type 2 diabetes for fifteen or twenty years, particularly those on insulin for many years, often have significant beta cell loss that cannot be reversed. This is the single biggest determinant of whether full remission is achievable. The mechanism for reversal exists. Whether the patient still has the biological substrate to express it depends on how long the disease has been progressing.
This is why early intervention matters disproportionately. A patient who arrives within two to four years of diagnosis is biologically very different from a patient who arrives after twenty years of progressive disease, multiple insulin injections daily, severe fatty liver, and advanced metabolic damage. Both can improve. The first is more likely to fully remit.
Clinical Perspective: What I See in Practice
The typical patient who arrives in my practice asking about reversal is already defeated. They have been in the medical system for years, sometimes decades. They have been told that diabetes is chronic, progressive, and irreversible. They have been managed — competently, often — but not investigated. The questions they have rarely heard are: why did this happen, can we remove the drivers, can we restore insulin sensitivity? The hidden message they received was that their body is broken and medication management is the future.
These patients typically arrive on some combination of metformin, a statin, blood pressure medication, sometimes a GLP-1 drug, and in more advanced cases insulin — often with progressively increasing doses over the years. Some are on five or six medications for what is fundamentally one disease. They have been told their HbA1c is “controlled” while their fasting insulin, TG/HDL ratio, and liver enzymes were never measured or were dismissed as secondary concerns. They feel resigned, often frustrated, and frequently somewhat skeptical that anything different is possible.
The conversation that opens possibility is simple. I ask: what if your diabetes is not a life sentence, but a reversible metabolic state — provided we address the conditions that created it? This single reframe moves the patient from disease identity to biological mechanism, and that is where hope begins. The body is not broken. It is responding adaptively to chronic conditions, and the conditions are addressable. From that frame, the rest of the work becomes possible.
The 12-week trajectory in patients whose biology responds well is recognizable enough that I describe it to patients in advance, so they know what to expect.
Week 1 is the rapid stabilization phase. Carbohydrates are reduced. The eating window is structured. Protein is increased. Night eating is removed. Sleep is anchored to a fixed wake time with morning light exposure. Within days, glucose variability drops on the CGM. Fasting glucose begins to fall. The first inflection point appears immediately: glucose often improves faster than expected, which means medications — particularly any sulfonylureas and any insulin — may already be too high for the new physiology. This is when the first GP coordination conversation happens. The risk of hypoglycemia during rapid improvement is real and has to be managed actively, not reactively.
Week 4 is the insulin unloading phase. Fasting glucose is clearly down. Postprandial spikes are blunted. Hunger and cravings reduce noticeably. Energy stabilizes. The first visible visceral fat reduction appears. Sulfonylureas are usually reduced or stopped by this point in responders. Insulin is often reduced stepwise. Metformin is typically continued through this phase. The inflection point at week 4 is the body shifting from glucose dependence toward improved fat oxidation — patients describe this subjectively as steadier energy, less need to eat frequently, and the disappearance of the post-meal energy crash that was previously normal for them.
Week 8 is the metabolic reprogramming phase. If we measure fasting insulin at this point, it is typically significantly lower. TG/HDL improves. ALT and GGT, the liver stress markers, improve. Sleep deepens. Cortisol rhythm stabilizes. Exercise capacity rises. Further insulin reduction or discontinuation occurs in responders. The GP is involved with regular glucose reporting. The inflection point at week 8 is hepatic insulin resistance starting to reverse — fasting glucose normalizes because the liver has stopped producing inappropriate glucose at inappropriate times.
Week 12 is the functional remission phase. Fasting glucose is near-normal. HbA1c is trending down — though as a 90-day rolling average, the full HbA1c improvement lags the fasting glucose improvement and continues to fall over the subsequent weeks even after the diet has stabilized the rest of the picture. Glucose variability is minimal. Appetite is regulated without effort. Visceral fat is clearly reduced. Many patients are off insulin by this point. Some reduce to metformin only or to no medications, depending on the case. The inflection point at week 12 is the system becoming self-regulating rather than compensatory — the patient is no longer fighting their diabetes. They have exited the metabolic state that created it.
The GP coordination piece runs through all twelve weeks and is critical. From week 1, the patient tracks glucose daily — finger-stick, CGM, or both. We establish structured communication with the GP, usually a weekly summary or shared log. The clear instruction to the patient and the GP is: medication must follow physiology, not the calendar.
The priority during rapid improvement is avoiding hypoglycemia, which is the real and immediate risk of starting metabolic intervention without medication adjustment. This is not a fight with the GP. Most GPs, when presented with declining glucose readings and a patient who is structurally improving, will adjust medications appropriately. The cases where this becomes adversarial are rare, and when they do, I help the patient find a more collaborative physician.
The patients I see across this trajectory are not engaging in willpower or discipline performance. They are giving the body a different set of inputs and watching the biology respond. The phrase I use with patients who reach week 12 is that they did not fight their diabetes. They exited the metabolic state that created it. The semantic difference matters because it accurately describes what happened — and because it changes how the patient understands their health for the rest of their life.
The Patients Who Do Not Fully Reverse
Not every patient reaches full remission, and the framing I give patients from the first consultation is honest about this. What I do not do is remove hope, because even partial reversal is a profoundly different long-term trajectory than the disease management framing would suggest.
Meaningful improvement without full remission can look like the following. HbA1c dropping from 9.2 percent to 6.4 percent. Insulin discontinued. Twenty to thirty kilograms of visceral fat loss. TG/HDL ratio normalized. Fatty liver markers improved. Stable energy and appetite. Major reduction in glucose variability on the CGM. Fewer medications and substantially better quality of life. None of this meets the technical definition of remission — the patient may still be on metformin, the HbA1c may still sit just above the diabetic threshold — but the biology is dramatically different from where they started, and the long-term complication risk is correspondingly different.
What determines whether a patient reaches full remission or reaches significant improvement without it comes down to a small number of variables. Duration of diabetes is the largest. Residual beta cell function. Degree of pancreatic exhaustion. Visceral fat burden at baseline. Sarcopenia and overall muscle mass. Sleep and circadian damage from years of disrupted physiology. Medication history, particularly long-term insulin use. Adherence consistency. And how early the intervention was initiated relative to the disease course.
A patient who arrives within four years of diagnosis with reasonable beta cell reserve, no significant sarcopenia, and consistent adherence will often reach full remission. A patient who arrives at twenty years post-diagnosis on multiple insulin injections daily, with severe fatty liver and advanced sarcopenia, will often achieve substantial improvement but not full remission. Both outcomes are worth pursuing. The framing I use is that even partial reversal massively changes long-term trajectory — it changes the rate of complication progression, the medication burden, the quality of life, and the metabolic resilience the patient carries forward.
I never promise cure. I explain that recovery exists on a spectrum, that the goal is restoring physiology rather than achieving a specific number, and that the work is worth doing regardless of where the patient lands on that spectrum. Patients need realistic hope — not fantasy, but also not the hopelessness they were previously given.
The Dietary Protocol I Actually Use
The dietary protocol differs in intensity between a freshly diagnosed type 2 diabetes patient and a fifteen-year insulin-dependent patient, but the foundation is consistent. The protocol is anchored in The Animal-Based Protocol for Insulin Resistance →, with adjustments calibrated to where the patient sits on the disease severity spectrum.
There is a set of day-one removals that applies almost universally regardless of patient profile. Sugar-sweetened beverages. Fruit juice. Refined flour in all forms. Breakfast cereals. Ultra-processed snack foods. Frequent grazing and snacking throughout the day. Nighttime eating. Industrial seed-oil-heavy processed foods. These removals alone can dramatically reduce glucose variability within the first week, often before any other dietary structure is added. For some patients, the day-one removals plus nothing else produce visible CGM improvement that is itself a teaching moment — the patient sees what their food choices have been doing to their glucose physiology and the abstract becomes concrete.
For a freshly diagnosed type 2 diabetes patient, the first four weeks typically follow a lower-carbohydrate animal-based whole-food approach. Protein-centered meals. Eggs, meat, fish, and Greek yogurt or raw dairy if tolerated. Some fruit depending on the individual glucose response, often introduced after the first two weeks. Optional root vegetables in metabolically healthier individuals.
Two to three meals per day, no grazing. A twelve-to-fourteen-hour overnight fasting window initially, expanding as adherence stabilizes. The carbohydrate target is typically around 50 grams per day, the protein target is approximately 1.6 grams per kilogram of ideal body weight, and dietary fat is the primary energy source. The goal is to lower insulin demand without overwhelming the patient psychologically. Many newly diagnosed patients improve rapidly with moderate carbohydrate restriction if adherence is high.
For a fifteen-year type 2 diabetes patient on insulin, the first four weeks are more therapeutic and more medically coordinated. The protocol is very low-carbohydrate initially. Animal-based emphasis. High protein. Nutrient-dense whole foods. Minimal glycemic load. Often temporary removal of most starches and fruits in the first weeks. No grazing. A compressed eating window introduced carefully, with hypoglycemia monitoring throughout.
The reason for the more aggressive initial restriction is that the goal in this population is rapid reduction in exogenous insulin requirement, hepatic glucose output, glucose variability, and hyperinsulinemia. These patients often respond dramatically — frequently more dramatically than newly diagnosed patients would expect — but they require closer monitoring because medications can become excessive quickly as physiology improves.
There is a meaningful distinction between active type 2 diabetes and earlier-stage insulin resistance in protocol design. Earlier insulin resistance patients have more metabolic flexibility, more carbohydrate tolerance, and broader food diversity is possible. Active type 2 diabetes patients have lost glucose-handling capacity, and the protocol initially has to be more “metabolically quieting” — fewer inputs that the system has to manage. As insulin sensitivity improves over the 12-week trajectory, flexibility often returns, and many patients reintroduce some carbohydrates from whole-food sources by week 8 or 12 without losing the gains.
The protocol works because it removes the load on a system that has been chronically overloaded. The body is not being engineered into a particular state. It is being given a substrate that allows it to return to a state it once occupied naturally.
The GLP-1 Question
The GLP-1 receptor agonists — semaglutide (Ozempic, Wegovy), tirzepatide (Mounjaro, Zepbound), and the newer generation drugs — are now common enough in the patient population that any honest discussion of type 2 diabetes reversal has to address them directly. My position is pragmatic, not ideological.
These drugs can produce meaningful short-term benefits. Appetite reduction. Weight loss. Lower glucose. Reduction in what patients describe as food noise — the constant cognitive presence of food and craving. Temporary metabolic stabilization. For some patients, particularly those with severe obesity or uncontrolled type 2 diabetes who have struggled to adhere to dietary intervention, GLP-1 drugs can create a therapeutic window that makes lifestyle restoration finally possible. The medication does work, and dismissing it ideologically would be clinically irresponsible.
What I do not view GLP-1 drugs as is a root-cause solution. The medication itself does not automatically restore circadian biology, food quality, muscle mass, mitochondrial function, stress physiology, metabolic flexibility, or the patient’s relationship with eating behavior. It produces appetite suppression and weight loss while it is being taken. It does not resolve the underlying metabolic dysfunction that produced the disease in the first place. When the drug is discontinued without foundational change, the metabolic dysfunction that was suppressed often re-emerges — sometimes faster than the patient or the prescriber anticipated.
My framework is straightforward: use the tool without mistaking the tool for the cure. In patients who respond well to GLP-1s, as visceral fat falls, fasting insulin improves, appetite regulation normalizes, muscle mass and activity improve, and glucose stabilizes, we typically discuss gradual dose reduction with the GP. Not every patient must discontinue immediately. Sometimes remaining temporarily on a low dose is clinically reasonable, particularly in patients with severe baseline obesity where the medication is enabling physical activity and resistance training that would otherwise be inaccessible.
I do not refuse to work with patients who stay on GLP-1 drugs. What matters is whether they are committed to the foundational work — restoring physiology, preserving and building muscle, improving sleep, improving diet quality, and rebuilding metabolic resilience. The patients I find clinically frustrating are not the ones using GLP-1s. They are the ones who view the drug as the answer and decline to engage with the underlying biology, because in those cases the medication is suppressing dysfunction without resolving it, and the long-term trajectory does not change.
There is one specific concern with GLP-1 drugs that deserves emphasis: muscle loss. A substantial fraction of weight lost on GLP-1 monotherapy is lean tissue, not fat. Skeletal muscle is the largest insulin-sensitive tissue in the body and a primary determinant of long-term glucose disposal. Patients who lose significant muscle mass on GLP-1s, particularly older patients and women, can end up metabolically worse off in the long term despite weighing less. Resistance training and adequate protein intake are not optional in patients on GLP-1 therapy. They are essential. This is one of the most actionable interventions I make with patients arriving on these drugs, and it is consistently underemphasized in conventional prescribing.
What I Watch For: Differential Diagnoses That Are Not Type 2 Diabetes
Before any reversal protocol begins, the differential diagnosis matters. Two specific conditions are often misdiagnosed as type 2 diabetes and require different management, and I screen for them in every new patient.
Latent Autoimmune Diabetes in Adults (LADA) is autoimmune destruction of beta cells presenting in adulthood, often diagnosed initially as type 2 diabetes because of the patient’s age. LADA does not respond to dietary intervention the way type 2 diabetes does, because the underlying mechanism is autoimmune, not metabolic. Antibody testing — GAD antibodies, IA-2 antibodies, and ZnT8 antibodies — distinguishes LADA from type 2 diabetes. A patient who looks like type 2 but does not have significant insulin resistance, who is lean, and who has not had the typical pre-diabetic trajectory, deserves antibody testing before anyone discusses reversal.
MODY (Maturity Onset Diabetes of the Young) is a group of monogenic diabetes conditions, typically with strong family history, presenting in younger patients without the typical type 2 diabetes risk profile. MODY responds to specific medications based on the genetic subtype and is not addressed by metabolic restoration in the same way.
These differentials are uncommon but not rare, and missing them produces patients who try a reversal protocol, do not respond, and conclude that nothing works. The diagnosis has to be correct before the protocol can be designed.
Documented Outcomes
The framework described in this post is not theoretical. The patients who have completed the 12-week protocol with documented outcomes include cases of HbA1c reversal from 10.5 percent to 6.2 percent in twelve weeks with insulin discontinued, HbA1c reversal from 9.2 percent to 6.5 percent in fourteen weeks with three medications reduced to one, and severe insulin resistance cases with fasting insulin moving from above 28 to below 10 µIU/mL within ten weeks. These outcomes are anonymized, consent-stated, and published in full on the documented outcomes page, where patients can see the labs, the timelines, and the protocol details for each case.
The point of presenting documented outcomes is not promotional. It is calibrative. Patients arriving with type 2 diabetes deserve to see what is realistically possible in their condition, with their level of disease severity, in the timeframe they are looking at. The cases on the documented outcomes page are not the average — they are individual patients with individual circumstances — but they are real, and they establish the upper bound of what is achievable when the protocol is followed consistently.
A Note on Uncertainty
The evidence base for type 2 diabetes remission through dietary intervention has grown substantially over the past decade. The DiRECT trial demonstrated that dietary intervention can produce remission in nearly half of patients within twelve months, with remission rates correlated to weight loss. The Virta Health studies have demonstrated similar outcomes with carbohydrate-restricted approaches. Multiple randomized trials and observational cohorts now support the basic premise that type 2 diabetes is, in many patients, a reversible condition.
What remains less precisely defined is the individual variability in who reaches full remission and who reaches significant improvement without remission. The variables are known — duration of disease, residual beta cell function, visceral fat burden, sleep and circadian status, sarcopenia, adherence — but the precise contribution of each variable to the individual outcome is not yet predictable in advance. Some patients respond more dramatically than the disease severity would predict. Some patients respond less. The protocol described in this post reflects what I have seen across years of practice and what is consistent with the published literature, but it does not promise outcomes for any individual patient.
The interventions described — dietary restructuring, sleep and circadian alignment, resistance training, medication coordination — are clinically established and safe when implemented with appropriate monitoring. Patients with established type 2 diabetes, particularly those on insulin or sulfonylureas, must coordinate any dietary or lifestyle changes with their treating physician to avoid hypoglycemia during rapid improvement. This post is educational and is not a substitute for individualized medical care.
People Also Ask
Can type 2 diabetes really be reversed permanently?
Type 2 diabetes can be put into remission — defined as HbA1c below 6.5 percent without glucose-lowering medication for at least three months — in a substantial fraction of patients, particularly those within the first few years of diagnosis. However, the underlying metabolic susceptibility does not vanish. A patient who achieves remission and returns to the dietary, sleep, and lifestyle pattern that produced their original diabetes will see the disease recur. Remission is the restoration of normal glucose regulation through restoration of underlying physiology, not a permanent cure.
How long does it take to reverse type 2 diabetes?
In patients whose biology responds well, the typical 12-week trajectory shows fasting glucose improvements within the first week, significant insulin reduction by week 4, hepatic insulin resistance reversal by week 8, and functional remission with normalized fasting glucose and trending HbA1c by week 12. HbA1c continues to fall for several weeks beyond the 12-week mark because it is a 90-day rolling average. Full remission status — confirmed by HbA1c below 6.5 percent without medication for three months — is typically established between weeks 16 and 24.
What is the most important factor in reversing type 2 diabetes?
The single largest determinant of whether full remission is achievable is residual beta cell function — meaning how much insulin secretion capacity the pancreas has retained. This is largely determined by duration of disease. Patients within the first few years of diagnosis typically retain substantial beta cell function and have higher remission rates. Patients with twenty or more years of progressive disease, particularly those on long-term insulin therapy, often achieve significant improvement but rarely full remission. Early intervention disproportionately matters.
Do you have to lose weight to reverse type 2 diabetes?
In most patients, yes — particularly visceral fat. Visceral fat and fatty liver are the central drivers of the insulin resistance that defines type 2 diabetes, and reducing them is typically essential to restoring insulin sensitivity. However, the focus is on restoring metabolic physiology, not on a number on the scale. Some patients reverse their diabetes with relatively modest total weight loss because the visceral and hepatic fat reduction is disproportionate to the total weight change. Body composition matters more than total weight.
Can you reverse type 2 diabetes if you are on insulin?
Yes, in many cases — but the protocol has to be more carefully coordinated with the prescribing physician because insulin doses become excessive quickly as the underlying biology improves, creating a real risk of hypoglycemia. Patients on long-term insulin who have severely depleted beta cell function may not achieve full remission, but substantial improvement with significant insulin reduction or discontinuation is common. Insulin therapy is not a barrier to attempting reversal, but it does change how the protocol is implemented.
Is the reversal of type 2 diabetes the same as remission?
Functionally, yes — the medical literature has converged on the term “remission” rather than “reversal” because it more accurately describes the clinical state. Remission means HbA1c below 6.5 percent without glucose-lowering medication for at least three months. The underlying metabolic susceptibility persists, which is why the term “cure” is not used. Both “reversal” and “remission” describe the same biological state — restoration of normal glucose regulation through correction of underlying physiology.
What is the role of GLP-1 drugs like Ozempic in type 2 diabetes reversal?
GLP-1 drugs can produce meaningful short-term benefits — appetite reduction, weight loss, glucose stabilization, and reduced food noise — and can create a therapeutic window in which lifestyle restoration becomes possible for some patients. However, the medication itself does not restore the underlying drivers of metabolic dysfunction. Used as a tool alongside foundational changes in diet, sleep, muscle preservation, and circadian alignment, they can be integrated into a reversal protocol. Used as a substitute for those changes, they suppress symptoms without resolving the disease, and the dysfunction typically re-emerges when the drug is discontinued.
About the Author
Morteza Ariana is a State-Certified Functional Nutritionist based in Germany, specializing in insulin resistance, type 2 diabetes, and root-cause metabolic restoration. He holds advanced training in systems-based physiology and has worked with patients across the U.S. and Europe for over 10 years.
His clinical framework is built around a core principle that mainstream medicine consistently overlooks: chronically elevated insulin — not blood glucose — is the earliest and most actionable driver of metabolic disease. That conviction was shaped in part by his own experience with hyperinsulinemia in 2016, and deepened through a decade of clinical practice and the study of leading researchers in metabolic medicine including Benjamin Bikman, Joseph Kraft, Gerald Reaven, Jason Fung, and Stephen Phinney.
His work focuses on identifying and correcting the upstream metabolic signals — insulin load, liver-gut axis dysfunction, circadian misalignment, and micronutrient gaps — that standard screening misses entirely. Patient outcomes are documented, anonymized, and published on this site.
If this resonates, the next step is clarity
The Metabolic Restoration Blueprint is a structured 12-week framework designed to correct upstream metabolic drivers — not just manage symptoms.
Key References
- Lean MEJ, Leslie WS, Barnes AC, et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. The Lancet. 2018;391(10120):541–551. 🔗 https://pubmed.ncbi.nlm.nih.gov/29221645/
- Lean MEJ, Leslie WS, Barnes AC, et al. Durability of a primary care-led weight-management intervention for remission of type 2 diabetes: 2-year results of the DiRECT open-label, cluster-randomised trial. Lancet Diabetes & Endocrinology. 2019;7(5):344–355. 🔗 https://pubmed.ncbi.nlm.nih.gov/30852132/
- Hallberg SJ, McKenzie AL, Williams PT, et al. Effectiveness and safety of a novel care model for the management of type 2 diabetes at 1 year: an open-label, non-randomized, controlled study. Diabetes Therapy. 2018;9(2):583–612. 🔗 https://pubmed.ncbi.nlm.nih.gov/29417495/
- Athinarayanan SJ, Adams RN, Hallberg SJ, et al. Long-term effects of a novel continuous remote care intervention including nutritional ketosis for the management of type 2 diabetes. Frontiers in Endocrinology. 2019;10:348. 🔗 https://pubmed.ncbi.nlm.nih.gov/31231311/
- Taylor R. Type 2 diabetes: etiology and reversibility. Diabetes Care. 2013;36(4):1047–1055. 🔗 https://pubmed.ncbi.nlm.nih.gov/23520370/
- Taylor R, Al-Mrabeh A, Sattar N. Understanding the mechanisms of reversal of type 2 diabetes. Lancet Diabetes & Endocrinology. 2019;7(9):726–736. 🔗 https://pubmed.ncbi.nlm.nih.gov/31097391/
- Riddle MC, Cefalu WT, Evans PH, et al. Consensus report: definition and interpretation of remission in type 2 diabetes. Diabetes Care. 2021;44(10):2438–2444. 🔗 https://pubmed.ncbi.nlm.nih.gov/34462270/
- Volek JS, Phinney SD, Krauss RM, et al. Alternative dietary patterns for Americans: low-carbohydrate diets. Nutrients. 2021;13(10):3299. 🔗 https://pubmed.ncbi.nlm.nih.gov/34684300/
- Westman EC, Yancy WS Jr, Mavropoulos JC, Marquart M, McDuffie JR. The effect of a low-carbohydrate, ketogenic diet versus a low-glycemic index diet on glycemic control in type 2 diabetes mellitus. Nutrition & Metabolism. 2008;5:36. 🔗 https://pubmed.ncbi.nlm.nih.gov/19099589/
- Wilding JPH, Batterham RL, Calanna S, et al. Once-weekly semaglutide in adults with overweight or obesity. New England Journal of Medicine. 2021;384(11):989–1002. 🔗 https://pubmed.ncbi.nlm.nih.gov/33567185/
- Jastreboff AM, Aronne LJ, Ahmad NN, et al. Tirzepatide once weekly for the treatment of obesity. New England Journal of Medicine. 2022;387(3):205–216. 🔗 https://pubmed.ncbi.nlm.nih.gov/35658024/
- Wilding JPH, Batterham RL, Davies M, et al. Weight regain and cardiometabolic effects after withdrawal of semaglutide: the STEP 1 trial extension. Diabetes, Obesity and Metabolism. 2022;24(8):1553–1564. 🔗 https://pubmed.ncbi.nlm.nih.gov/35441470/
- Bikman BT, Mavropoulos JC, Westman EC. Insulin resistance and type 2 diabetes: a review. Nutrients. 2020;12(10):2954. 🔗 https://pubmed.ncbi.nlm.nih.gov/32987684/
- Unwin DJ, Tobin SD, Murray SW, Delon C, Brady AJ. Substantial and sustained improvements in blood pressure, weight and lipid profiles from a carbohydrate restricted diet: an observational study of insulin resistant patients in primary care. International Journal of Environmental Research and Public Health. 2019;16(15):2680. 🔗 https://pubmed.ncbi.nlm.nih.gov/31357547/
- Naude CE, Brand A, Schoonees A, et al. Low-carbohydrate versus balanced-carbohydrate diets for reducing weight and cardiovascular risk. Cochrane Database of Systematic Reviews. 2022;1(1):CD013334. 🔗 https://pubmed.ncbi.nlm.nih.gov/35088407/
- American Diabetes Association Professional Practice Committee. Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Supplement 1). 🔗 https://pubmed.ncbi.nlm.nih.gov/38078589/
