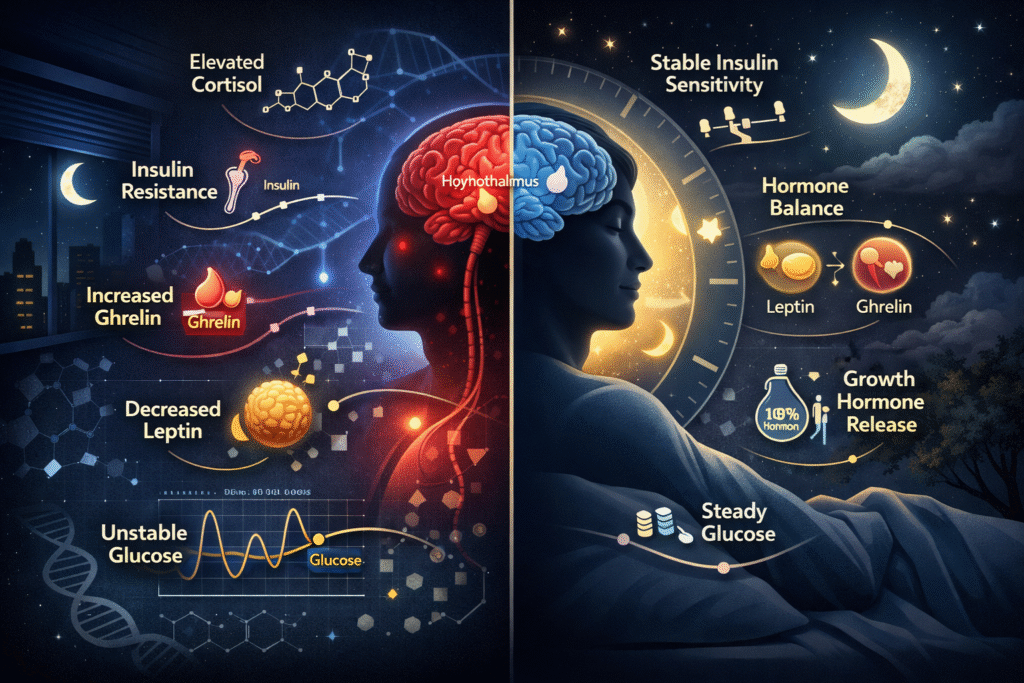
A metabolic reality many high-performers and even clinicians underestimate
Sleep Affects Metabolic Health
are tightly connected through hormones, circadian rhythms, and glucose regulation. When sleep is consistent and sufficient, metabolic processes stay balanced—but sleep deprivation can disrupt insulin sensitivity, appetite hormones, and blood sugar control.
Over the years I have worked with many people who are extremely disciplined. Entrepreneurs, physicians, engineers, athletes—individuals who are used to solving problems through effort.
When their metabolism starts to drift in the wrong direction—rising fasting glucose, stubborn fat gain, fatigue, poor recovery—the first instinct is usually the same:
Improve the diet. Train harder. Add discipline.
Often they succeed in doing exactly that. Nutrition becomes cleaner. Training becomes more structured. Supplements are added. Intermittent fasting or carbohydrate restriction might be introduced.
And yet something strange happens.
Despite all the effort, the metabolic needle barely moves.
Whenever I encounter this pattern, I start investigating one variable very carefully: sleep.
What I repeatedly observe is that many high performers treat sleep as negotiable. It becomes the first biological function sacrificed in the pursuit of productivity.
But physiology does not treat sleep as optional.
From a metabolic perspective, sleep is not merely recovery time. It is one of the primary regulators of energy balance, glucose control, and hormonal stability.
When sleep is chronically compromised, the body begins to operate under altered neuroendocrine conditions.
And under those conditions, diet and exercise lose much of their metabolic effectiveness.
Conclusion:
Sleep is not simply rest. It is a core regulator of metabolism, and ignoring it undermines even the best diet or training program
Sleep Restriction Creates Insulin Resistance
When clinicians discuss insulin resistance, the conversation usually revolves around nutrition, physical inactivity, or excess body fat.
Those factors are certainly important. But sleep deprivation alone can produce significant changes in insulin signaling.
Controlled sleep laboratory studies have demonstrated that restricting sleep to 4–5 hours per night for about a week can reduce insulin sensitivity by roughly 20–30 percent.
This magnitude of impairment is comparable to what we observe in early metabolic syndrome.
Several mechanisms contribute to this effect.
Elevated cortisol
Sleep restriction shifts the circadian rhythm of cortisol. Instead of declining in the evening, cortisol levels remain elevated, promoting hepatic glucose production and antagonizing insulin action.
Sympathetic nervous system activation
Chronic sleep loss increases sympathetic tone, pushing the body into a stress-dominant physiological state that favors glucose release rather than glucose storage.
Reduced peripheral glucose uptake
Muscle tissue—the largest sink for glucose disposal—becomes less responsive to insulin under sleep-deprived conditions.
The result is a predictable pattern: glucose remains elevated longer after meals.
In the era of continuous glucose monitoring, I see this phenomenon frequently.
Even individuals with excellent nutrition can experience noticeably worse glucose control after a night of poor sleep.
The diet did not change.
The regulatory environment did.
Conclusion:
Sleep deprivation alone can produce meaningful insulin resistance — even in otherwise healthy individuals.
Appetite Regulation Is Neurological, Not Just Behavioral
Another powerful effect of insufficient sleep occurs in the regulation of appetite.
Hunger is not governed purely by conscious choice. It is regulated by a complex hormonal and neurological network designed to maintain energy balance.
Two hormones are particularly important in this system:
- Leptin, which signals satiety
- Ghrelin, which stimulates hunger
Sleep restriction alters both.
Studies consistently show that inadequate sleep leads to lower leptin levels and higher ghrelin levels.
The brain interprets this hormonal pattern as a signal of energy deficiency.
As a result, appetite increases.
But the shift goes beyond simple hunger.
Sleep deprivation also enhances activation of reward circuits in the brain, particularly in regions involved in food motivation. Individuals begin to crave energy-dense foods, especially those high in carbohydrates and seed oils.
From an evolutionary perspective, this makes perfect sense. If an organism experiences sleep disruption, the brain may interpret this as environmental stress and attempt to increase energy intake.
In the modern food environment, however, this biological response can easily lead to excessive caloric intake.
Many people interpret these cravings as a failure of discipline.
In reality, they often reflect neurobiological changes triggered by insufficient sleep.
Conclusion:
Sleep deprivation alters hunger hormones and brain reward pathways, biologically increasing appetite and food cravings.
Training Cannot Replace Recovery
Among highly motivated individuals, there is often an assumption that increased training can compensate for poor sleep.
Physiology does not support this assumption.
Exercise is a powerful metabolic stimulus. But it is also a physiological stressor that requires adequate recovery to produce adaptation.
Sleep is the primary window in which that recovery occurs.
Several important processes depend on sufficient sleep.
Growth hormone release
Deep sleep is associated with pulses of growth hormone, which supports tissue repair, fat metabolism, and recovery from physical stress.
Testosterone production
Research has shown that restricting sleep to about five hours per night for one week can reduce daytime testosterone levels in healthy men by approximately 10–15 percent.
Inflammation control
Sleep deprivation increases inflammatory markers such as IL-6 and C-reactive protein, which interfere with recovery and metabolic regulation.
In practice, individuals who train intensely while sleeping poorly often experience a familiar pattern:
- stalled fat loss
- persistent fatigue
- reduced training performance
- slower recovery
Adding more training rarely solves the problem. In fact, it often compounds the physiological stress load.
The system simply lacks the biological environment necessary for adaptation.
Conclusion:
Exercise stimulates metabolic improvement, but sleep enables recovery and adaptation. Without sleep, training cannot deliver its full benefit.
Circadian Rhythm: The Overlooked Metabolic Regulator
Sleep is not only about duration. Timing matters as well.
Human physiology follows a circadian rhythm—an internal biological clock largely synchronized by light exposure.
Many metabolic processes are influenced by this rhythm, including insulin sensitivity, hormone secretion, and energy metabolism.
Insulin sensitivity, for example, generally follows a daily pattern.
It tends to be higher earlier in the day and declines toward the evening.
When sleep schedules become irregular—late nights, inconsistent wake times, exposure to artificial light late at night—the alignment between circadian biology and behavior begins to deteriorate.
Shift work research illustrates this clearly.
Long-term night-shift workers show significantly higher risks of:
- type 2 diabetes
- obesity
- cardiovascular disease
Even when calorie intake is similar to daytime workers.
The mismatch between biological timing and behavioral patterns appears to disrupt metabolic regulation.
This is one reason I emphasize sleep consistency when working with individuals experiencing metabolic dysfunction.
Regular sleep timing stabilizes circadian signals and restores biological predictability.
And physiology functions best when those signals are predictable.
Conclusion:
Metabolic health depends not only on sleep quantity but also on maintaining a stable circadian rhythm.
What I Consistently Observe in Practice
When metabolic progress stalls, sleep is often the missing variable.
I have seen individuals struggle for months despite improving their nutrition and exercise routines. Yet when sleep duration improves—from five or six hours to closer to eight hours—metabolic markers begin to shift.
Fasting glucose stabilizes.
Energy improves.
Fat loss begins again.
Nothing else changed.
The diet was already good.
The training program was already structured.
What changed was the physiological environment in which metabolism operates.
Once the brain regained sufficient recovery time, hormonal and metabolic regulation began to normalize.
This does not mean diet and exercise are unimportant. They remain central components of metabolic health.
But they operate within the biological framework created by sleep.
When that framework is compromised, metabolic interventions often produce disappointing results.
Conclusion:
Restoring sleep often unlocks metabolic improvements that diet and exercise alone cannot achieve.
Final Thoughts
Modern health culture focuses heavily on two levers: nutrition and exercise.
Both matter enormously.
But neither operates in isolation.
Sleep influences multiple regulatory systems simultaneously:
- insulin sensitivity
- appetite control
- hormonal balance
- inflammatory signaling
- circadian alignment
When sleep is consistently inadequate, these systems drift out of balance.
No diet can fully override that disruption.
No training program can permanently compensate for it.
Discipline alone cannot defeat altered physiology.
For clinicians and high performers alike, the message is straightforward:
If metabolic health is the goal, sleep must be treated as a primary intervention.
Because biology follows its own rules.
And one of the most fundamental is this:
You cannot out-diet or out-train bad sleep.
People Ask Also
Can poor sleep really affect blood sugar and insulin sensitivity?
Yes. Even a few nights of restricted sleep can reduce insulin sensitivity and impair glucose tolerance. Research shows the body temporarily behaves metabolically similar to early insulin resistance when sleep becomes chronically insufficient.
Why do people crave unhealthy foods when they are sleep deprived?
Sleep deprivation alters appetite hormones. Ghrelin increases while leptin decreases, which raises hunger and strengthens cravings for calorie-dense foods like sugar and refined carbohydrates.
Can exercise compensate for poor sleep?
No. Exercise stimulates metabolic adaptation, but sleep is when the body repairs tissue, regulates hormones, and restores energy systems. Without sufficient sleep, much of the metabolic benefit of training is reduced.
How much sleep is generally needed for metabolic health?
Most adults require about 7–9 hours of consistent sleep per night. Both insufficient sleep and irregular sleep timing can disrupt hormonal regulation and impair glucose metabolism.
Does improving sleep help metabolic health?
Yes. Improving sleep duration and circadian rhythm can enhance insulin sensitivity, stabilize appetite regulation, and support better metabolic recovery, often unlocking progress when diet and exercise alone have stalled.
About the Author
Morteza Ariana is a State-Certified Functional Nutritionist based in Germany, specializing in insulin resistance, type 2 diabetes, and root-cause metabolic restoration. He holds advanced training in systems-based physiology and has worked with patients across the U.S. and Europe for over 10 years.
His clinical framework is built around a core principle that mainstream medicine consistently overlooks: chronically elevated insulin — not blood glucose — is the earliest and most actionable driver of metabolic disease. That conviction was shaped in part by his own experience with hyperinsulinemia in 2016, and deepened through a decade of clinical practice and the study of leading researchers in metabolic medicine including Benjamin Bikman, Joseph Kraft, Gerald Reaven, Jason Fung, and Stephen Phinney.
His work focuses on identifying and correcting the upstream metabolic signals — insulin load, liver-gut axis dysfunction, circadian misalignment, and micronutrient gaps — that standard screening misses entirely. Patient outcomes are documented, anonymized, and published on this site.
If this resonates, the next step is clarity
The Metabolic Restoration Blueprint is a structured 12-week framework designed to correct upstream metabolic drivers — not just manage symptoms.
Scientific References
Spiegel K., Leproult R., Van Cauter E. (1999) Impact of Sleep Debt on Metabolic and Endocrine Function – The Lancet
Buxton OM et al. (2010) Sleep Restriction for 1 Week Reduces Insulin Sensitivity in Healthy Men – Diabetes
Buxton OM et al. (2012) Adverse Metabolic Consequences in Humans of Prolonged Sleep Restriction Combined with Circadian Disruption – Science Translational Medicine
Donga E. et al. (2010) A Single Night of Partial Sleep Deprivation Induces Insulin Resistance in Multiple Metabolic Pathways in Healthy Subjects – Journal of Clinical Endocrinology & Metabolism
Potter G. et al. (2016) Circadian Rhythm and Metabolic Disease – Endocrine Reviews